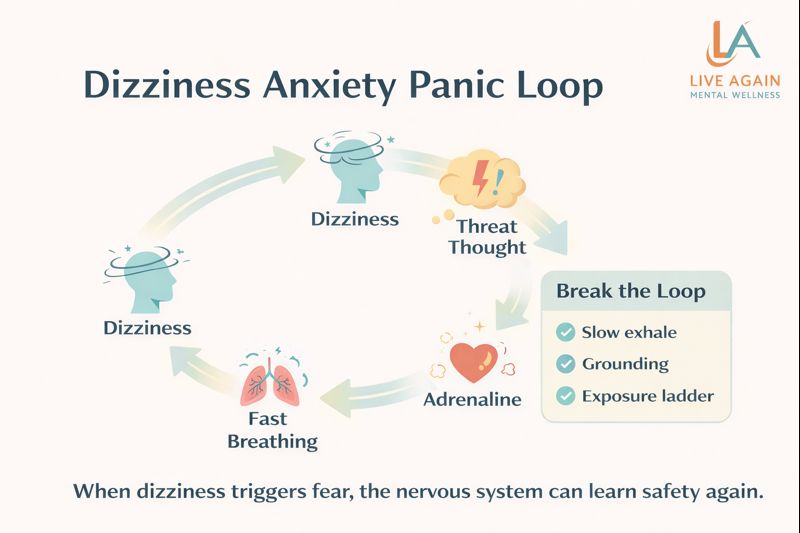
Dizziness Anxiety Panic Loop: When Dizziness Turns Into Panic
Dizziness Anxiety Panic Loop describes a common pattern: a brief sensation of giddiness gets labelled as danger, the body releases adrenaline, and the adrenaline creates more dizziness, breathlessness, and fear. Over time, the fear starts attaching to places (roads, traffic signals, markets) and situations (being alone, travelling, standing in queues). The good news is that this loop is learned—so it can be unlearned with the right plan. NHS – Anxiety, fear and panic
First rule: confirm medical safety without getting stuck in testing
Dizziness is a broad symptom. It can be linked to dehydration, low blood sugar, anemia, BP fluctuation, thyroid imbalance, inner‑ear/vestibular issues, medication side effects, sleep loss, or stress. If dizziness is new, persistent, worsening, or comes with neurological red flags (weakness, slurred speech, confusion), do a medical review first—because good therapy works best when the body is medically stable. After that, use the medical check as an anchor, not a repeated reassurance ritual. Mayo Clinic – Panic attacks (symptoms & causes)
Red flags that need urgent care
Seek urgent medical evaluation if dizziness comes with chest pain, fainting, severe shortness of breath, one‑sided weakness, speech changes, sudden severe headache, new seizure, or sudden hearing loss. These are not “wait and see” symptoms. If none of these are present, and dizziness rises mainly during fear situations, the nervous system pathway becomes a stronger suspect. NHS – When to go to A&E
How the Dizziness Anxiety Panic Loop starts in the brain
The brain is a prediction machine. When it cannot quickly explain a body sensation, it scans for threat and tries to “solve” it with the most alarming story: What if I faint? What if I die? What if I lose control in public? That catastrophic interpretation is the switch that turns discomfort into panic physiology. The moment fear joins the sensation, adrenaline rises—heart rate increases, muscles tighten, breathing changes—and the body starts to feel even stranger. NIMH – Panic disorder: when fear overwhelms
Not all dizziness is the same
People use “dizziness” as one word, but the body uses it in many ways: light‑headedness (like you might faint), vertigo (spinning), and disequilibrium (unsteady balance). Anxiety most commonly produces light‑headedness and “floating,” especially when breathing gets fast and shallow; vestibular conditions can produce true spinning vertigo; dehydration and low sugar can create faintness. Mapping your sensation accurately helps you choose the right action: medical review for persistent vertigo, hydration/meal correction for metabolic triggers, and anxiety skills for fear‑linked giddiness. Cleveland Clinic – Panic attacks & panic disorder
The learning mechanism: fear + place = a new danger map
If you felt dizzy at a traffic signal and panicked, the brain stores a simple rule: “signal = danger.” Next time, even anticipating the signal can trigger symptoms. You avoid that route, then you avoid travel, then you avoid leaving home alone. Avoidance reduces anxiety short‑term, which teaches the brain that avoidance is protective—so the map expands and life space shrinks. NHS – Agoraphobia overview
Safety behaviours that quietly keep fear alive
Safety behaviours look helpful, but they keep the brain from learning safety. Common examples: constant accompaniment, repeated BP/oxygen checks, sitting down immediately, scanning exits, carrying “just in case” items without a plan, calling family repeatedly, refusing to stop at signals, or cancelling social events. The mind concludes: “I survived because of the safety behaviour,” not “I survived because I was never in real danger.” We reduce these behaviours gradually, not abruptly—because the goal is sustainable independence, not a sudden shock to the system. NHS – Panic disorder
What’s happening in your body during a panic surge: Dizziness Anxiety Panic Loop
Dizziness Anxiety Panic Loop is powered by predictable physiology. Adrenaline changes breathing and blood chemistry; many people start breathing faster and shallower without realising it. When carbon dioxide drops, you can feel tingling, light‑headedness, blurred vision, and a floating sensation. This is why dizziness often increases after fear begins. It can feel extreme, but it is a body alarm system—uncomfortable, not fatal. Understanding the physiology reduces the fear and shortens the episode. NHS Greater Glasgow & Clyde – Panic disorder
The 90‑second reset: what to do when dizziness spikes
When dizziness spikes, the aim is not to “force it away,” but to signal safety to the nervous system. Use this 4‑step reset:
- Name it: “This is an anxiety surge, not a medical emergency.”
- Breath pace: inhale 4, exhale 6, for 10 cycles (slow exhale downshifts arousal).
- Anchor eyes: look at one stable object and describe it (shape, colour, edges) to shift attention outward.
- Release muscle alarm: drop shoulders, soften jaw, loosen hands.
Practise daily when calm, so the steps become automatic under stress. APA – Cognitive Behavioral Therapy (CBT)
Build an exposure ladder: small practice beats big battles
Exposure is the evidence‑based way to retrain fear. You approach what you avoid in small, repeated steps until the brain learns: “I can handle this.” Create a ladder that fits your current capacity:
- Doorstep for 2 minutes (no phone reassurance)
- Walk 50–100 metres and return
- Walk to a shop, stay 2 minutes, return
- Short car ride in a familiar lane; one planned stop
- Stop at a signal; stay through the discomfort; do the reset
- Increase distance: 3 km → 6 km → 10 km, with planned practice stops
The rule: stay until anxiety drops even a little (for example, 8/10 to 6/10). That drop teaches the brain. NHS – Agoraphobia treatment
Interoceptive exposure: training your body sensations
Many people fear the sensations themselves. Interoceptive exposure gently recreates sensations in a controlled way so the brain learns “these feelings are safe.” Examples (do only after medical clearance and start mild): brisk walking for 60–90 seconds to raise heart rate; turning in place slowly for 10 seconds to create mild dizziness; and practising slow exhale breathing to reverse breath‑panic patterns. The goal is not to suffer—it is to practise staying present until the sensation settles. This reduces fear of dizziness itself, which is the core fuel of panic loops. PMC – CBT in the treatment of panic disorder
Reduce body triggers that imitate panic
Caffeine, nicotine, dehydration, irregular meals, poor sleep, and late‑night scrolling can all increase palpitations, light‑headedness, and shakiness—making the nervous system easier to trigger. Stabilise basics: hydration, consistent meals with protein, moderate caffeine, and a fixed sleep window. These steps do not “cure” anxiety, but they reduce the number of false alarms your body sends to the brain—so your exposure practice becomes easier and safer. NHS – Anxiety and panic attacks
Family support that heals without creating dependency
Family love is a strength, but “rescuing” can become accidental training in dependency. A healthier model is support + coaching. Instead of repeating reassurance (“Nothing will happen”), use a coaching script:
- “Rate your fear 0–10. We will stay until it drops by 2 points.”
- “Let’s do the breathing together.”
- “We will follow today’s ladder step—no skipping, no forcing.”
This protects the client’s dignity and reduces caregiver burnout. Mind – Panic attacks
How first-degree family members get affected
When one member is trapped in avoidance, the whole household reorganises around fear—family members may stop travelling, avoid guests, or stay on constant alert. Over months, caregivers can develop irritability, insomnia, compassion fatigue, and even anxiety symptoms of their own. Naming this impact is not blame; it is reality. A family plan should include caregiver rest, role-sharing, and clear boundaries so support remains sustainable. WHO – Mental disorders
Work, travel, and functional impairment: plan your comeback
Panic-linked dizziness often creates “functional impairment”: missed workdays, reduced travel, avoidance of meetings, and fear of being alone in public. A practical comeback plan is graded return: start with short, predictable tasks; schedule one small exposure before work (like a 10‑minute walk); and use the 90‑second reset during symptoms rather than leaving immediately. Recovery is not only symptom reduction—it is life restoration, step by step. NHS Inform – Panic self-help guide
When anxiety pulls you into depression: Dizziness Anxiety Panic Loop
Long‑term avoidance shrinks life—and a shrunk life often creates depression: low energy, hopelessness, loss of interest, sleep disruption, and reduced confidence. If you notice these symptoms, treat depression alongside anxiety; otherwise exposure becomes harder. Behavioural activation (routine + small mastery tasks) is a practical way to restart reward signals in the brain. WHO – Depression
A simple weekly progress scorecard: Dizziness Anxiety Panic Loop
Track progress like rehabilitation, not like a test. Each week record:
- Time you can stay alone (minutes → hours)
- Distance you can travel
- Number of avoided situations you faced (even small)
- How many reassurance checks you reduced
- Sleep window consistency
This turns recovery into data, and data builds confidence. NIMH – Depression
Dizziness Anxiety Panic Loop recovery: three commitments for 6–8 weeks
Dizziness Anxiety Panic Loop improves when you commit to three non‑negotiables:
- One medical anchor: complete check‑up and follow advice; avoid repeating tests for reassurance.
- One exposure step daily: small, frequent practice (10–20 minutes) beats occasional long attempts.
- One boundary on reassurance: replace checking with skills (breathing, grounding, planned exposure).
Relapses are normal—treat them as “practice days,” not proof of failure. APA Monitor – Panic disorder treatment progress
A final clarity check: panic cycle, medical issue, or both?
Many clients have a mixed picture: a medical sensitivity (BP/thyroid/vestibular) plus anxiety amplification. If symptoms reduce with grounding and follow predictable fear triggers, anxiety is likely a major driver. If symptoms are new, progressive, or neurological, medical evaluation stays central. The best plan respects both realities and avoids the extremes of “it’s only medical” or “it’s only anxiety.” NHS – Panic disorder
Dizziness Anxiety Panic Loop: what recovery looks like in real life
Recovery is not “never feeling dizzy again.” Recovery is: you notice dizziness, you label it correctly, you use skills, and you continue the task without escaping. Over weeks, the episodes shorten; your routes expand; your confidence returns. The nervous system learns that discomfort is survivable—and that learning is the opposite of panic. NHS Inform – Panic self-help guide
Dizziness Anxiety Panic Loop: How therapist can help you
Dizziness Anxiety Panic Loop can recover faster when a therapist builds your exposure hierarchy, identifies and reduces safety behaviours, and trains panic‑recovery skills in real time. A therapist also supports your family in shifting from rescue to coaching, and treats depression (routine, sleep, motivation) alongside anxiety work. Most importantly, therapy gives a structured plan and accountability until your confidence becomes stable. Psychology Tools – Understanding panic
Welcome to Live Again India
Welcome to live again.
Live again India mental wellness is supporting you — you are not alone.
If fear has made your world small, we will help you expand it step by step, safely and respectfully.
Your life is precious, and recovery is possible with the right plan and consistent care.
L@A