
Emotional Clarity Big Decisions
Big decisions don’t need urgency-they need stability. When emotions rise, the brain shifts into survival mode and choices become extreme. Use a simple sequence: Regulate → Reflect → Decide, and delay irreversible steps for 24–72 hours unless safety is at risk. With calm structure and support, you can choose from strength, not from fear.

Stay Calm and Consistent
A calm, practical guide for all ages-learn a 60‑second reset, the 3 Anchors, and a daily minimum plan to stay steady without forcing positivity.

Anger and Communication Skills
Anger becomes destructive when the nervous system takes over and communication turns into attack or shutdown. Regulate first, speak one clean boundary, and use time‑out with a return time. Replace blaming and repeated checking with structure – check‑in windows, response rules, and repair within 24 hours. When safety becomes behavioural, respect and connection return naturally.

Overthinking and Decision Paralysis: 3‑Step Decision Protocol
Overthinking is not intelligence—it is anxiety disguised as responsibility. Use the 3‑step protocol (Clarify → Choose → Commit) to stop endless reopening. Decisions require structure, not perfection, and progress builds confidence. If fear and avoidance keep returning, treat it clinically—your nervous system may need retraining.
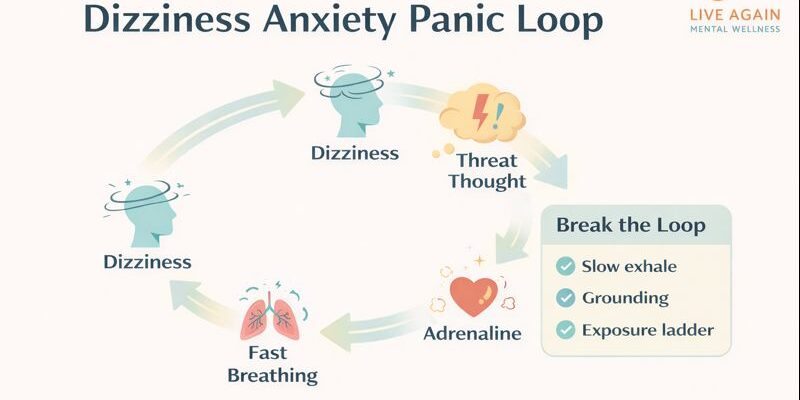
Dizziness Anxiety Panic Loop
Dizziness can feel like a medical emergency, but for many people it becomes an anxiety–panic feedback loop driven by fear and adrenaline.
A sudden body sensation triggers a threat interpretation, which spikes arousal, tightens breathing, and amplifies light-headedness.
The goal is not to “fight” dizziness, but to retrain safety through slow exhale, grounding, and graded exposure to avoided situations.
With consistent CBT-style practice, the brain learns: “This sensation is uncomfortable, not dangerous”—and the loop weakens.

Generalized Anxiety Disorder Help
Generalized Anxiety Disorder Help starts when you stop treating worry as “thinking” and start treating it as a nervous-system threat loop.
GAD is persistent, hard-to-control worry with tension, fatigue, poor focus, and sleep disruption—often across health, performance, and future risks.
CBT works by correcting threat predictions, reducing safety behaviours, and building tolerance for uncertainty through structured exposure and practice.
With a stable routine, sleep protection, and guided therapy, your mind regains flexibility—and life stops being organised around fear.

Bipolar disorder substance use
Bipolar disorder is highly sensitive to sleep and routine, and alcohol/cannabis can destabilize that rhythm even when they feel calming.
The most common relapse pathway is: short relief → sleep disruption → irritability/impulsivity → mood episode → increased substance use.
Family members are affected through chronic hypervigilance, conflict cycles, and caregiver burnout—so treatment must include the home system.
Recovery becomes realistic when you treat it as dual diagnosis: protect sleep, track patterns, reduce harm, and follow an integrated plan with a clinician.

Decision Fatigue: When Small Choices Start Feeling Heavy
Decision fatigue is a capacity signal, not a character flaw: when cognitive load stays high, the brain becomes risk-avoidant and choices start to feel costly.
It shows up as delay, overchecking, impulsive shortcuts, and a growing sense that even small decisions “take too much.”
The correction is not more willpower—it is better design: reduce options, create defaults, close open loops, and choose a daily Top-3.
When the body downshifts and the day has structure, clarity returns naturally—because the mind finally has space to breathe.
L@A


